CARDIOVASCULAR
DISEASE
Innovations in Clinical Trials and Hybrid Trials in Cardiovascular Disease
Better understanding of the role of remote patient monitoring in attenuating and improved care in cardiovascular disease has fueled a paradigm shift in cardiovascular clinical trials. While critical endpoints still require in clinic testing and imaging, the importance of electronic patient reported outcomes (ePRO) has changed the landscape for cardiovascular clinical trials. Through use of hybrid trial designs and electronic patient diaries more closely tracking symptoms, use of medication, monitoring vitals and dietary shifts, at SPRIM Health we can track these critical factors in real-time or near real time. This significantly transforms understanding of disease progression and drug effectiveness. It also enables intervention to occur every day in a standardized and digital capacity and course correct sooner. Such technology-enabled solutions help to prevent large deteriorations in clinical course, while patients wait for periodic clinical visits and recall is blurred.
Wearables and Biosensors
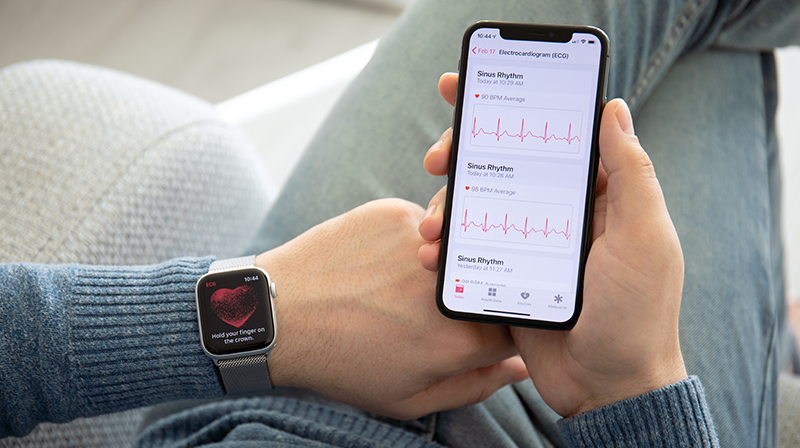
There are now many FDA approved wearable and biosensor devices that can accurately detect and monitor vitals such as heart rate, blood pressure, temperature, body weight and oxygen saturation. In addition to these basic parameters, at SPRIM Health, we have successfully implemented and integrated more robust cardiac sensors such as 6 lead ECGs. For heart failure patients, with accurate and integrated ways to monitor parameters such symptoms, diet, and body weight, it becomes possible to intervene before cardiac function incurs significant irreversible declines. In addition, use of remote patient monitoring through at home blood pressure measurements has been proven to significantly improve blood pressure control and management of hypertension, which are two of the leading causes of stroke.
More Compliance and Data Accuracy Using Digital Training
Digital training and education can greatly improve data quality in cardiovascular clinical trials. Digital patient training is recommended by the FDA as the leading factor that can improve and optimize the quality of a clinical trial. As such the FDA PRO Guidance (2009) asserts that “standardized instructions and processes that can appear in the protocol should include training and instructions to patients for self-administered PRO instruments”. Digital patient training in cardiovascular studies is generally focused on an overview of the trial, patient roles and responsibilities, expectation setting, honesty and accuracy in reporting, video vignettes on how to use wearables and/or biosensors, the importance of compliance with symptoms, diet and medication tracking and how to report any changes in health status.
Symptoms Tracking via Patient eDiaries
SPRIM Health has considerable expertise in developing and validating novel ediaries for both chronic and acute cardiovascular diseases (tracking symptoms, diet and medication use). It is also critical to program algorithms to remotely monitor patients for significant changes in health status and to develop an escalation pathway if symptoms cross specific thresholds within a certain period of time. Such methodology is relevant for all phases of cardiovascular clinical trials. By collecting more complete and better data quality in phase I and II studies, improves the probability of success to get to a phase III study and a more reliable approval. There are new technologies for data collection enabling standardized data collected across phases (ePROs on patients own smartphones, wearables (i.e., FDA-approved ECGs and blood pressure cuffs) biosensors, biospecimen kits for home use, telehealth visits, use of central labs and central raters). There is a changing landscape in cardiovascular clinical trials from getting patient data at a point in time (clinic visit) vs daily and/or continuous data stream in real-time/near real time via ePRO and technology enabled strategies.
More Accurate Collection of AEs
In cardiovascular disease, early detection of adverse events is critical. Digitized capture of potential AEs and SAEs can significantly improve safety signal quality. Research has shown that patients report symptoms/AEs earlier and more frequently than clinicians detect them and that clinicians systematically downgrade patient symptom severity. Using an app on a patient’s smartphone can enable daily and episodic collection of both solicited and unsolicited potential AEs. Patients can bidirectionally communicate with dedicated virtual site clinical staff using live chat, phone calls and email messaging to triage shifts in health status and synchronize with physical sites as needed.